Through efforts led by LE&RN (the Lymphatic Education & Research Network), the Senate has passed a bill for the LD Commission (Lymphatic Disease Commission) to increase research and lymphatic education. The bill passed in the Senate last month, with a vote of 68-31. Now that it’s passed in both houses of Congress, it is now on President Biden’s desk to be signed into law. This is exciting and unprecedented news for men and women suffering from lymphatic diseases!
Video: LE&RN’s Appeal to Congress video here.
The following language is taken directly out of the recently passed bill and is a direct reflection of the hard work and dedication of advocates in this community. NHLBI refers to the National Heart, Lung, and Blood Institute and NIH refers to the National Institute of Health, two of the nation’s medical research agencies that support scientific studies for advancing knowledge and discovery in health.
Lymphedema (LE)—The agreement directs NHLBI to increase support for research on LE and to establish a Research Condition Disease Categorization category for research related to lymphedema.
National Commission on Lymphatic Diseases—The agreement directs NIH to establish a National Commission on Lymphatic Diseases and to engage with relevant Institutes, Centers, and external stakeholders in establishing this Commission. The agreement directs NIH to provide an update on progress to establish the Commission within 60 days of the enactment of this Act.

Why is Passing the Lymphatic Disease Education Bill So Important?
This is the latest step in pushing for resources for deeper research into the causes, best treatment practices, and even genetic dispositions for lymphatic diseases that are not yet clearly identified across healthcare. A National Commission on Lymphatic Diseases pushes Lymphatic Diseases to the forefront of national research as a priority, and ultimately this gives experts in this field a seat at the table to tell Congress what we need in order to provide the best care to patients. Most exciting, the bill now directs NIH to establish this Commission within the next two months after President Biden signs!
Takeaways from the bill:
- Establishment of a research category for Lymphatic Diseases:
- Once NIH establishes a category for Lymphatic Education, there will be no more uncertainty about their level of research or commitment in this area. The 2022 bill directs NIH to create this category of research. Previously, Lymphatic disease research essentially “fell through the cracks” of medical research without belonging to a category.
- Request for greater funding and support:
- The Bill clearly then asks for an increase in Lymphatic Education research funding.
- Another LE&RN agenda item that is included in the 2022 bill is a doubling of funding for the CDC’s Chronic Disease Awareness Grants.
- LE&RN received a three-year grant from this program in 2021 to pursue a Lymphatic Education Awareness Campaign. This new funding secures the program.
Understanding Lymphedema Diseases
Lymphedema is a condition that occurs when lymphatic fluid, a transparent liquid composed of fat, water, salts, and proteins, begins to pool and accumulate in the arms and the legs. The initial and most predominant symptom indicating the presence of Lymphedema is significant swelling of these extremities. Medical experts point to damaged lymph vessels as the cause of fluid retention leading to Lymphedema. When lymphatic fluid isn’t able to properly circulate through the human bloodstream via lymph nodes and vessels, retention quickly occurs. Other potential causes for fluid retention are linked to infections, genetics or underlying medical conditions especially cancer and its treatment. Keep reading to learn more about the treatment of Lymphedema in St Louis.
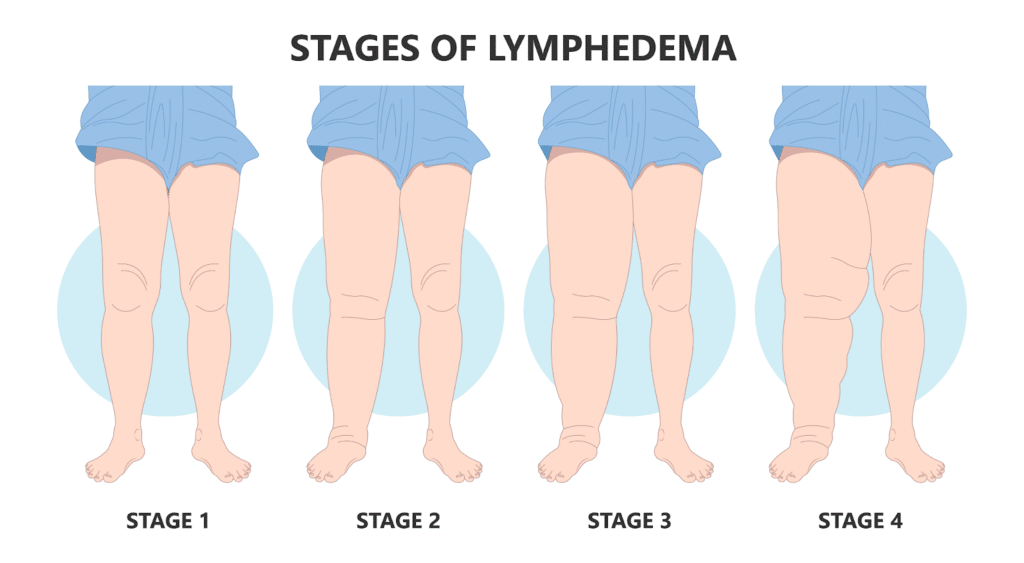
Types of Lymphedema
It is widely understood and accepted that Lymphedema can be an inherited medical condition and as a result, is recognized under three distinct categories. Congenital Lymphedema refers to symptoms that develop in early childhood. Lymphedema Praecox refers to symptom development that occurs during adolescence, while Lymphedema Tarda refers to symptoms that show up in patients later in life. Lymphedema quite commonly develops in patients as a result of a traumatic injury damaging lymphatics. This type of trauma is generally linked to the removal of lymph nodes during surgical procedures related to cancer treatment or radiation. Infection is a second factor closely linked to the development of Lymphedema.
Skin Lymphostatic Fibrosis
This is a widespread side effect in patients with lymphedema, where the skin hardens over time. In the early stages of lymphedema, swelling is soft to the touch. However, over time, the swelling hardens the skin due to the development of connective tissue fibers underneath the skin of the affected areas.
Papillomatosis
The growth of numerous papillomas, more commonly referred to as warts.
Dermal Sclerosis
Hardening and tightening of the skin and connective tissues.
Leg Swelling
Leg swelling is one of the most common symptoms of lymphedema and prompts patients to seek treatment.
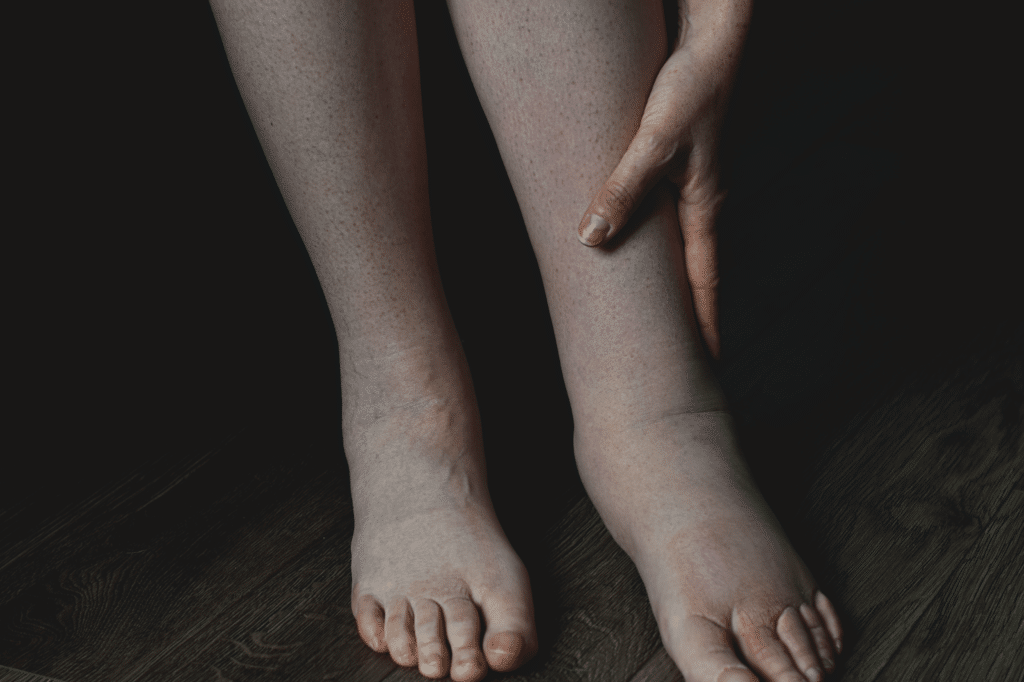
Lymphedema is a progressive condition that can quickly transform into a more serious medical issue. The risks of leaving Lymphedema untreated can include a heightened vulnerability to infection leading to lymphangitis and cellulitis. Similarly, Lymphedema can commonly lead to fibrosis or hardening and scarring of the skin and subcutaneous fat cells. This condition has the potential to impede the overall circulation of lymph fluid causing physical movement to become a painful task. These conditions comprehensively increase the pressure put on veins working to move blood through the body towards the heart.
Diagnosis Prior to Treatment
A physical exam will be carried out and the results compared to the patient’s medical history and profile. A venous doppler ultrasound is commonly utilized to assess the potential for venous insufficiency which can also lead to increased swelling of the limbs. To verify the presence of Lymphedema, a physician may choose to perform a Lymphoscintigraphy. This procedure involves the injection of a radioactive solution into the potentially affected area of the body to decisively map the path of lymphatic fluids in a targeted region. The option for the physician to perform a Lymphangiography involves the replacement of the radioactive solution with a medicinal dye.
Home Care Strategies
Patients suffering from Lymphedema are at a greater risk of developing infections and there are some simple home care strategies that help diminish the overall risk factor. Those suffering from Lymphedema should always completely dry affected limbs after showering or swimming. Wearing protective shoes and clothing reduces the risk of cuts or injuries while the addition of compression garments is highly recommended in the promotion of healthy blood circulation. Sitting with the legs uncrossed is another simple strategy towards promoting improved lymphatic flow. Maintaining a dedicated exercise routine along with a healthy diet has been shown to help reduce the risk of injury or infection related to Lymphedema.
Seeking Lymphedema Treatment
While there is no permanent cure for Lymphedema, complications, and progression of the disease can be managed effectively with a combination of Lymphedema treatment St Louis options. Compression garments are the primary method recommended for managing Lymphedema. Compression stockings, sleeves, leggings, and gauntlets provide the first line of defense when it comes to promoting healthy blood circulation. Manual lymphatic drainage or massage can aid in the management of Lymphedema as well. This technique works to manually move the lymph out of congested areas. When this type of massage is combined with compression bandages the treatment method may be referred to as Complete Decongestive Therapy.
For patients with more severe cases of Lymphedema, intermittent compression pump lymphedema therapy may prove effective. These compression pumps actively work to move trapped lymphatic fluid through the lymphatic circulatory system.